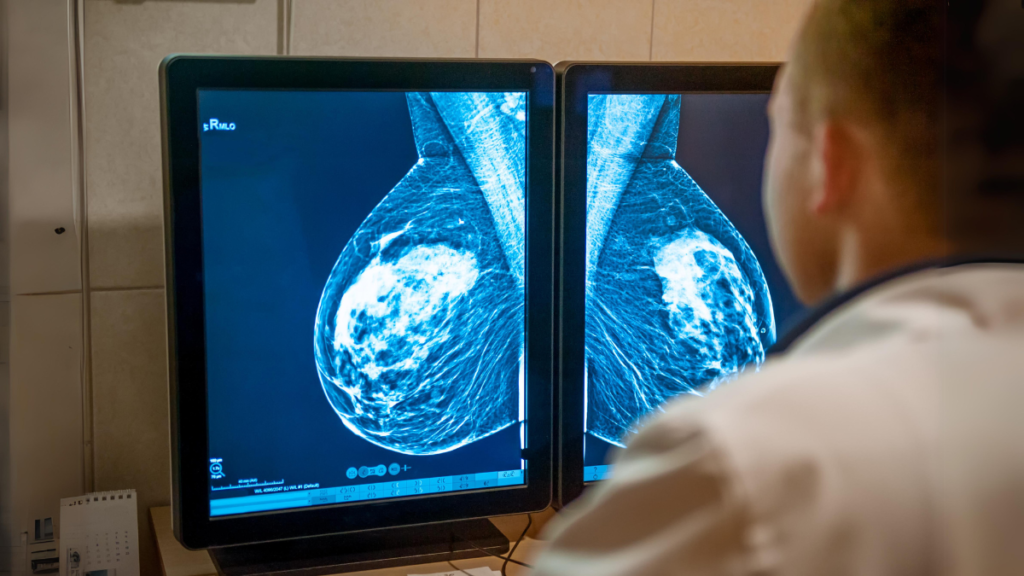
October is the Breast Cancer Awareness Month in UK.
- With increasingly more women enquiring about breast cancer screening, where do doctors stand?
- Should we or should we not offer early breast cancer screening?
- Is evidence and assessing the pros and cons of an early mammogram enough to deter a younger woman who wishes to ensure she does not have breast cancer, or that breast cancer is detected early?
Current Breast Screening Programmes
NHS Breast Cancer Screening traditionally has started at the age of 50 and has been undertaken until a woman turned 70. However the NHS is currently rolling an extension programme with breast cancer screening starting at the age of 47 until the age of 73.
With most breast cancers being sporadic and not associated with a family history, should we offer women breast cancer screening at an earlier age?
It is generally accepted that offering breast screening every 12-18 months to women from the age of 40 is correct practice for those who wish to be proactive and are able to support the associated costs. The potential benefit from early cancer screening is considered to outweigh the small risk from radiation exposure that occurs with each mammogram.
Investigations Being Used In Breast Cancer Screening
Digital Mammography with computer-aided detection is currently considered the gold standard in breast cancer screening. They are proven to be better at picking up breast cancers in women with high breast density that a traditional film mammography.
A 3D Mammography is a type of digital mammogram also called Breast Tomosynthesis. The radiation dose is slightly higher than a 2D Mammography. This is available at private clinics across UK, although the precise advantages have not been made entirely clear to date. Is currently seen as another tool in identifying breast cancers.
Many women in our clinics enquire about breast MRI. The value of breast MRI in detecting cancers remains uncertain at present, with some doctor advocating that MRI is better at picking up abnormal breast tissue than the mammography. However due to reduced availability of breast MRI and higher associated costs, breast MRI tends to be reserved currently for situations such as:
- Second line assessment of abnormal breast findings
- Investigating a woman who has a palpable abnormality but mammogram and/ or ultrasound is normal
- Evaluation of high density breasts
- Evaluation of the breast tissue in women with silicone breast implants
- Evaluation of a cancer spread
Breast Density
Not all clinics report on the density of a breast following a mammogram.
In USA, several states made it a legislative requirement that a woman is informed of her breast density following a mammogram. This is because every 1% increase in breast density is linked with a 2% increased risk of breast cancer. In addition, the accuracy of a mammogram is lower the higher the breast density. Of note is that half of women, who present with breast cancer within 1 year of a negative screening mammogram, have above average breast density.
Women who have been informed that have increased breast density should be made aware of a higher risk of developing breast cancer and that undertaking an ultrasound along with the mammogram increases the chance of detecting an early breast cancer.
Breast Cancer Screening in Pregnancy
Women’s breasts undergo significant changes whilst pregnant. These changes may make it more difficult to detect breast cancer.
An ultrasound is considered a safe investigation for women who are pregnant. A mammogram may also be carried out if indicated.
Breast Cancer Screening in Breastfeeding Mothers
Although generally breastfeeding reduces the risk of breast cancer, lower risk does not mean zero risk. Although most lumps are related to lactation issues, it is rare but some women do develop breast cancer during the lactation period
Breastfeeding should not stop a woman or a healthcare professional proceeding to breast cancer screening.
Breastfeeding women should undertake mammography, and is generally recommended that the breasts be emptied before the procedure. An ultrasound may also be recommended for these patients.
Breast Cancer Screening in women with Breast Implant
Breast implants may decrease the ability of detecting breast cancers. However this should not deter women.
Mammograms in women with implants include four additional views, so called ‘implant displacement views’.
In some cases a breast MRI may also be recommended.
Our Approach
We, at ROC Clinic, encourage all women to be aware of breast cancer screening and regularly examine their breasts for lumps.
We offer all women screening mammograms from the age of 40, every 12-18 months. We may start breast screening earlier than age 40 and in such cases we may recommend a breast ultrasound or a breast MRI too.
If you are unsure whether or not you should start breast screening, you should discuss it with your doctor. Breast screening for cancer may start as early as age 30, provided all the pros and cons have been discussed, along with any other genetic cancer screening such as BRAC1 and BRAC2.
If you wish to discuss it with one of our doctors, why don’t you contact us today! Learn more about our One-Stop Breast Clinic.

